Foot care is essential if you have diabetes because the condition damages nerves and reduces blood flow to your feet. This combination makes you vulnerable to unnoticed injuries, slow-healing wounds, and serious infections that can lead to amputation. Daily foot inspections, proper washing, moisturizing, and wearing protective footwear can prevent life-threatening complications. With diabetic foot ulcers affecting 12% of patients and causing 80% of non-traumatic amputations, understanding proper care techniques could save your limbs.
Key Takeaways
- Diabetes causes nerve damage in 50% of patients, reducing sensation and ability to detect foot injuries.
- Foot ulcers affect 12% of diabetic individuals and lead to 80% of non-traumatic lower limb amputations.
- Daily foot inspections can identify early warning signs like cuts, blisters, or redness before they become serious.
- Poor circulation from diabetes slows healing, making even minor foot injuries potentially dangerous.
- The five-year mortality rate after a foot ulceration is around 30%, highlighting the severity of these complications.
The Growing Problem of Diabetic Foot Complications
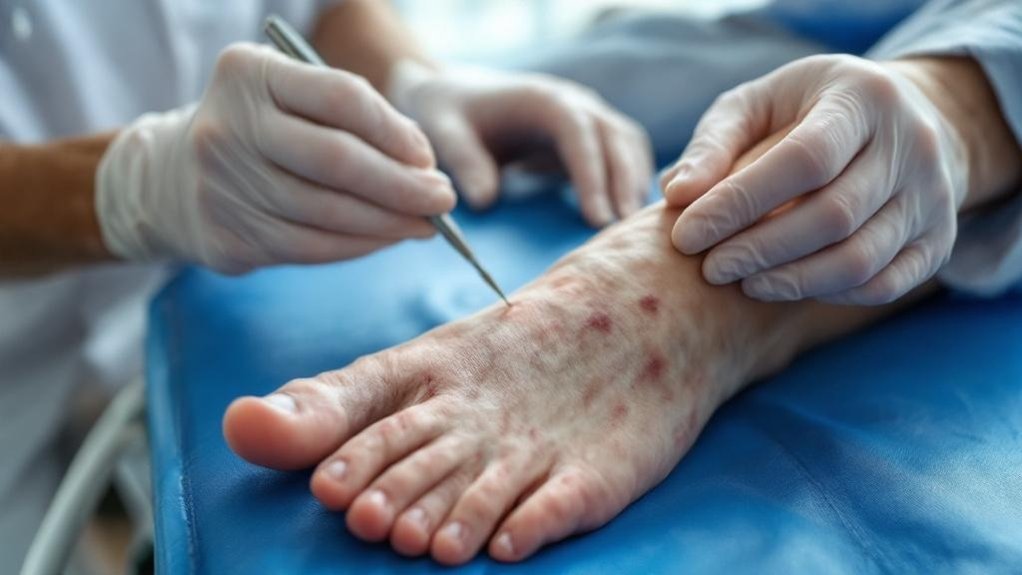
While diabetes impacts multiple body systems, foot complications represent one of its most devastating consequences. You’re facing a significant risk—approximately 12% of people with diabetes develop foot ulcers during their lifetime, with the global prevalence reaching 6.3% of all diabetic adults.
The economic burden is substantial, with prolonged hospitalizations and intensive treatments straining healthcare systems worldwide. If you’re living with diabetes, you should know that foot ulcers lead to 80% of non-traumatic lower limb amputations, and the five-year mortality rate following ulceration approaches 30%. Recent research shows that diabetic foot ulcers have recurrence rates reaching up to 65% over a five-year period.
Regional variations exist, with North America seeing rates of 13.0% compared to 5.5% in Asia. You’re part of a community facing this challenge together, making prevention and early intervention vital to your long-term health.
Understanding How Diabetes Affects Your Feet
Diabetes creates five critical pathways that compromise foot health, fundamentally altering how your body protects and heals this vulnerable area. Nerve damage (neuropathy) reduces sensation, making injuries go unnoticed in nearly 50% of patients. You’ll experience tingling, burning, or complete numbness, preventing you from feeling dangerous cuts or pressure points.
Simultaneously, reduced blood flow impairs healing and oxygen delivery. This dangerous combination leads to structural deformities like claw toes and Charcot foot, creating new pressure points where ulcers develop. Your immune system’s weakened response means infections progress rapidly—contributing to the 130,000+ annual amputations in the U.S. Additionally, skin changes including dryness and cracking create entry points for bacteria. Daily foot inspections are essential for early detection of these problems before they become severe. Understanding these interconnected threats is your first defense against serious complications.
Warning Signs That Require Immediate Attention
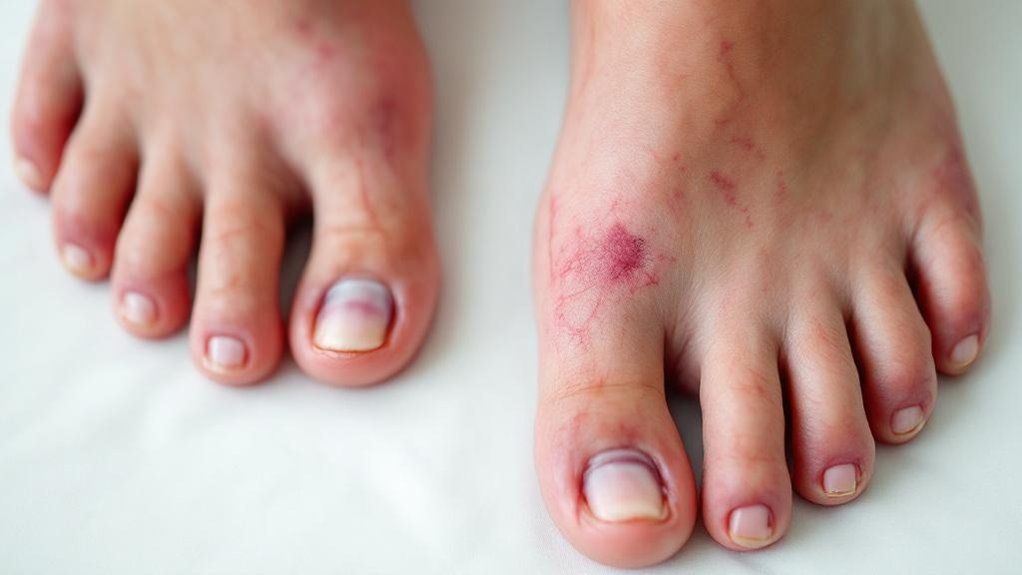
Recognizing danger signals in your feet can mean the difference between successful treatment and serious complications like amputation. Be vigilant for numbness symptoms like tingling, “pins and needles,” or loss of sensation, as these indicate nerve damage that prevents you from feeling injuries.
Watch for infection signs including redness, swelling, warmth, or drainage from wounds. Any pus, foul odor, or unexplained fluid on your socks demands urgent care. Continuous glucose monitoring with reliable sensors can help you remain proactive by identifying trends that might contribute to poor wound healing or increased risk of infections. Pain while walking or resting, especially when it develops suddenly, shouldn’t be ignored.
Also monitor for structural changes like unusual foot shape or “rocker bottom” deformities, which signal advanced complications. Remember, you’re not alone—half of all diabetic patients experience peripheral neuropathy. Early detection and prompt medical attention are essential for preserving your foot health. Slow-healing sores require immediate medical attention as they represent a critical warning sign of potential complications in diabetic patients.
Daily Foot Care Practices That Save Lives
Implementing a thorough daily foot care routine can dramatically reduce your risk of serious complications from diabetes. Start with daily inspections, carefully examining every part of your feet for cuts, blisters, or redness—especially between toes where problems often begin unnoticed.
Wash your feet daily with lukewarm water, never hot, and dry gently between each toe. Apply moisturizing techniques to prevent cracking, but avoid placing lotion between toes where fungal infections thrive. Always wear protective footwear, even indoors, and choose seamless socks that won’t create pressure points. Consistent monitoring of your blood sugar levels is essential to preventing diabetes-related foot problems.
Trim toenails straight across and file edges smooth. Remember that consistent care isn’t just about prevention—it’s about being part of a community that prioritizes health and independence through simple, life-saving habits.
Health Disparities and Risk Factors in Diabetic Foot Care

While diabetes affects millions of Americans, its complications don’t impact all communities equally. Health inequities greatly influence diabetic foot outcomes, with African Americans experiencing higher rates of ulcers and amputations than White individuals. These disparities persist even in higher-income groups.
Your risk factors include diabetes duration, delayed treatment, and foot infections. Living in economically disadvantaged or rural areas can further compromise your access to specialized care, worsening outcomes. Limited health literacy may also hinder effective diabetes management.
Socioeconomic constraints often force delayed medical interventions, while systemic healthcare barriers create additional challenges. Understanding these disparities is vital for addressing gaps in care and ensuring everyone receives appropriate preventative foot care, regardless of race, location, or economic status. The risk of developing diabetic foot ulcers is significant, with approximately 19% to 34% of diabetes patients experiencing this complication during their lifetime.
Frequently Asked Questions
Can Special Socks Improve Circulation in Diabetic Feet?
Yes, proper diabetic socks can enhance circulation in your feet. Mild compression promotes blood flow while specialized sock materials minimize friction and wick moisture—key elements in protecting your diabetic feet from complications.
How Do Weather Changes Affect Diabetic Foot Health?
Temperature fluctuations can worsen circulation and neuropathy symptoms in your diabetic feet. Seasonal moisture increases infection risk, while extreme heat or cold may damage skin. Always adapt your foot care to weather changes.
Are Certain Exercise Types Safer for Diabetic Feet?
Yes, low-impact activities are safest for your diabetic feet. Choose pool walking, recumbent cycling, or tai chi, and always wear proper diabetic footwear with cushioning to protect vulnerable pressure points.
Do Medicare/Insurance Plans Cover Specialized Diabetic Footwear?
Yes, Medicare Part B covers your custom footwear needs, including one pair of shoes annually plus inserts. Your supplemental insurance may help with the 20% coinsurance Medicare doesn’t cover.
Can Foot Care Products With Natural Ingredients Replace Medicated Options?
While natural remedies like honey and aloe vera offer ingredient benefits for mild conditions, they shouldn’t completely replace medicated options for diabetic foot care. Consult your healthcare provider about integrating both approaches.
Conclusion
You can’t afford to ignore your feet when you have diabetes. They’re uniquely vulnerable to complications that can escalate rapidly. By checking your feet daily, wearing proper footwear, maintaining glucose control, and seeking prompt medical attention for any changes, you’re taking crucial steps to prevent serious complications. Remember, proactive foot care isn’t optional—it’s a critical component of your diabetes management plan.
