Diabetes greatly impacts skin health, affecting 30-80% of patients through multiple pathways. We see manifestations like diabetic dermopathy, acanthosis nigricans, and increased susceptibility to bacterial and fungal infections due to hyperglycemia’s suppression of immune function. Advanced glycation end-products damage skin structure while microvascular impairment reduces nutrient delivery, creating characteristic symptoms. Tight glycemic control remains the cornerstone of prevention alongside targeted topical treatments. The complex interplay between metabolism and dermatological health reveals much about diabetes progression.
Key Takeaways
- Diabetes affects skin health in 30-80% of patients through conditions like diabetic dermopathy, acanthosis nigricans, and increased vulnerability to infections.
- Hyperglycemia impairs immune function and promotes bacterial growth, making diabetic patients more susceptible to skin infections and delayed wound healing.
- Advanced glycation end-products damage skin structure, reducing elasticity and increasing dryness through compromised microvascular integrity.
- Effective skin management requires glycemic control, proper moisturization, and regular screening for early identification of complications.
- Preventive strategies include consistent blood glucose management, thorough skincare routines, and prompt attention to any skin changes.
The Diabetes-Skin Connection: Understanding the Prevalence

While the prevalence of skin manifestations in diabetic patients varies across studies, we’re consistently seeing that cutaneous complications affect between 30-80% of individuals throughout their disease course. This wide variation stems partly from insufficient patient education, with over 50% of physicians failing to inform patients about potential skin complications.
The data reveals concerning patterns: Type 2 diabetes patients represent 85% of skin manifestation cases, typically presenting in their 50s to 60s. Specific conditions like diabetic dermopathy affect up to 30% of patients, particularly those with elevated glycosylated hemoglobin levels. Infectious complications are the most prevalent among diabetic patients with skin manifestations.
We believe regular skin screening should be standard practice, especially for those with longstanding diabetes. By recognizing these metabolic-dermatological connections early, we can help you maintain both glycemic control and skin integrity as integral parts of your diabetes management.
Common Skin Manifestations in Diabetic Patients
Although diabetes primarily affects blood glucose regulation, its metabolic disruptions manifest prominently on the skin, creating visible markers of the disease’s progression. We often observe diabetic dermopathy—brownish spots on the shins—as the most prevalent cutaneous sign, indicating compromised microcirculation and reduced skin hydration.
Acanthosis nigricans presents as velvety dark patches in body folds, signaling insulin resistance. In many patients, we note diabetic thick skin, particularly on extremities, where impaired moisture retention leads to waxy textures. Prompt detection of necrobiosis lipoidica can prevent progression from small reddish-brown spots to larger waxy patches on the shins.
The appearance of painless diabetic bullae (blisters) represents a rare but diagnostically significant manifestation. While some lesions resolve within two years with optimized glucose control, others persist indefinitely. Our clinical experience confirms that maintaining metabolic balance remains essential for skin integrity.
Bacterial and Fungal Infections: Why Diabetics Are More Susceptible
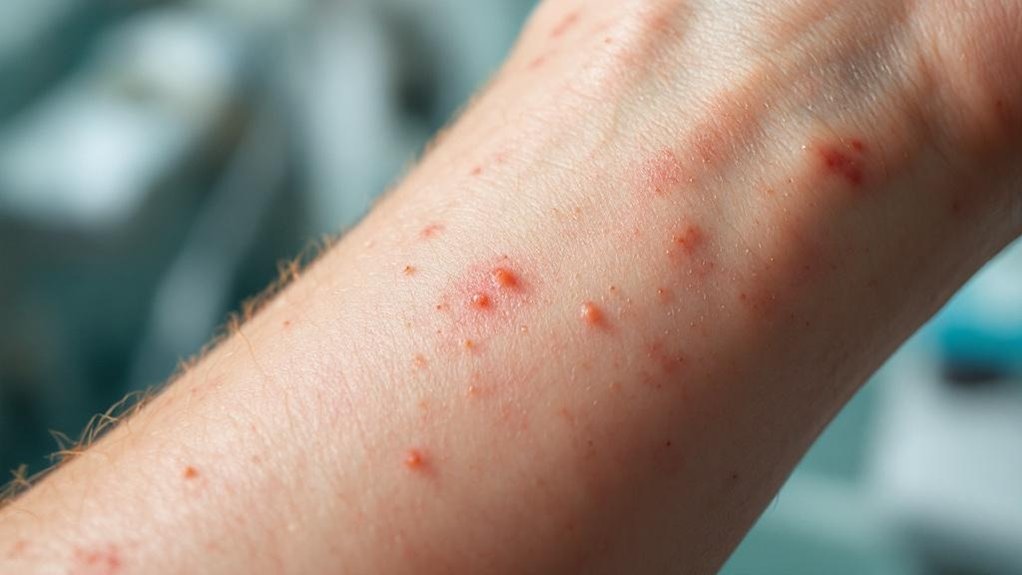
Because of their compromised immune function and altered tissue environment, diabetic patients face considerably higher risks of bacterial and fungal skin infections than the general population.
We observe multiple factors creating this vulnerability. First, hyperglycemia directly suppresses leukocyte function while simultaneously providing ideal conditions for bacterial overgrowth and fungal colonization. The glucose-rich environment fundamentally serves as a pathogen feeding ground. These infections often appear as part of the skin manifestations range that can indicate poor glycemic control in diabetic patients.
Additionally, vascular impairments reduce vital blood flow to potentially infected areas, limiting both immune cell delivery and effective antibiotic distribution. The combination of neuropathy (reducing sensation of early infection) and compromised skin barrier function creates perfect entry points for opportunistic pathogens.
For our diabetic community members, recognizing these physiological challenges is essential. Understanding why your body responds differently to pathogens empowers you to implement more effective preventative skin care strategies.
Recognizing Diabetic Dermopathy and Its Characteristics
Diabetic dermopathy manifests as asymptomatic, reddish-brown atrophic lesions primarily on the shins, affecting approximately 50% of individuals with diabetes due to vascular compromise and impaired wound healing mechanisms. We must differentiate these “shin spots” from age spots, dermatitis, or trauma-induced hyperpigmentation by noting their bilateral distribution, well-demarcated borders, and association with other microvascular complications. While no specific treatment eliminates diabetic dermopathy, maintaining ideal glycemic control and applying high glycerine-based moisturizers can improve appearance as these lesions typically resolve spontaneously over time. Patients should be aware that these lesions are usually a centimeter or less in size and rarely cause discomfort or irritation.
Shin Spots Appearance
Recognizing shin spots, medically known as diabetic dermopathy, requires attention to their distinctive visual presentation. These characteristic shin lesions typically manifest as round or oval patches with a shiny, scar-like appearance, measuring under 1 centimeter but occasionally reaching 2.5 centimeters.
We find these lesions initially present with pink, tan, or purple hues before maturing to reddish-brown or dark brown tones. The skin pigmentation changes occur mainly on the anterior shins bilaterally, though they may also develop on thighs, feet, and forearms. You’ll notice these spots feature a subtle central depression and often appear in clusters rather than isolated lesions.
Most patients with diabetic dermopathy won’t experience itching, burning, or fluid discharge from these patches, which become smoother as they mature. These skin manifestations are particularly common, affecting approximately 50% of diabetics who develop some form of skin disease during their lifetime.
Diagnosis vs. Other Conditions
When evaluating suspicious skin lesions on the shins, we’ll need to distinguish diabetic dermopathy from several similar-appearing conditions through careful clinical assessment. The diagnostic criteria primarily involve identifying non-blanching, scaly macules or papules (1-2.5cm) with a characteristic bilateral but asymmetric distribution.
In our differential diagnosis, stasis dermatitis requires particular attention as it commonly mimics diabetic dermopathy. We look for the progression from red-purple lesions to atrophic, depressed scars—a hallmark transformation that occurs over approximately two years. While biopsies are typically avoided due to poor wound healing concerns in diabetic patients, histopathological features like epidermal atrophy, collagen fragmentation, and hemosiderin deposition provide definitive confirmation when necessary. The presence of at least four classical lesions is considered diagnostic for diabetic dermopathy and should prompt investigation for potential underlying microvascular complications.
Treatment Options Available
Although diabetic dermopathy typically resolves without intervention, establishing ideal glycemic control remains our primary therapeutic strategy. We recognize that insulin regulation directly impacts keratinocyte function, making blood sugar control essential for skin health.
For topical management, we recommend retinoids, vitamin D analogs, and moisturizers containing urea or ammonium lactate. These address thickened skin areas while providing symptomatic relief. The light brown, scaly patches characteristic of diabetic dermopathy commonly appear on the shins of patients.
In our practice, we’ve observed promising results with holistic approaches that complement medical interventions. Some patients benefit from dietary supplements like alpha-lipoic acid and omega-3 fatty acids that support cellular metabolism.
For persistent cases, we may consider advanced options including laser therapy, pentoxifylline for improved circulation, or localized corticosteroid injections. Together, we’ll develop a personalized treatment plan addressing your specific manifestations.
Physiological Mechanisms Behind Diabetic Skin Conditions
We’ll now examine how protein glycation drives functional and structural changes in diabetic skin, where advanced glycation end-products disrupt cellular processes and compromise microvascular integrity. The hyperglycemic environment triggers cascading damage to skin vasculature, with endothelial dysfunction and basement membrane thickening contributing to compromised nutrient delivery and waste removal. These vascular changes, coupled with macrophage dysfunction and altered inflammatory responses, create the perfect storm for the characteristic skin manifestations observed in poorly controlled diabetes. Additionally, subclinical skin inflammation contributes significantly to diabetic dermatopathy development before visible symptoms appear.
Glycation’s Cellular Impact
At the cellular level, glycation triggers a cascade of destructive processes that fundamentally alter skin structure and function in diabetic patients. When blood glucose levels remain elevated, AGEs actively generate and accumulate in tissues, creating profound glycation effects on skin cells.
We’ve observed that glycated collagen becomes highly resistant to degradation by matrix metalloproteinases, markedly retarding normal turnover. This collagen damage manifests as fragmentation of fibers, severely compromising structural integrity. The resulting cross-links become virtually impossible to repair, leaving skin less elastic and more prone to wrinkling.
Additionally, keratinocytes and fibroblasts—essential for wound healing—experience functional impairment in high glucose environments, accelerating cellular senescence. This microenvironment disrupts cell-matrix interactions, altering cellular adhesion and growth patterns that we rely on for healthy skin maintenance. The interaction between AGEs and RAGE receptors activates inflammatory signaling pathways, including NF-κB and MAP kinase, further exacerbating skin damage in diabetic patients.
Microvasculature Damage Cascade
Beneath the surface of diabetic skin complications lies a complex microvasculature damage cascade that’s driven by sustained hyperglycemia. We observe how prolonged elevated glucose levels directly damage the small blood vessels responsible for nourishing skin tissues. This microvascular dysfunction creates a domino effect, compromising oxygen and nutrient delivery to dermal cells.
In our patients, we note how these vascular changes manifest alongside skin barrier deterioration. The increased trans-epidermal water loss we measure correlates with clinical presentations of xerosis and impaired wound healing. When small vessel damage progresses, we see the activation of inflammatory pathways involving IL-6 and TNF-alpha. The accumulation of advanced glycation end-products further contributes to skin structure alterations and reduced elasticity in diabetic patients. Together, we’re witnessing how these cascading effects alter collagen structure and compromise dermal integrity—creating the foundation for many diabetic dermatological manifestations we treat daily.
Immune Response Alterations
Diabetes considerably alters immune responses throughout the body, creating a perfect storm of physiological changes that manifest in skin complications. When hyperglycemia persists, we observe significant immune dysfunction characterized by weakened pathogen resistance and altered inflammatory markers.
The diabetic state often leads to chronic inflammation that dysregulates normal immune cell behavior. This impairs the skin’s protective mechanisms, making you more vulnerable to common infections like Staphylococcus aureus. High blood glucose levels provide an ideal environment for bacterial proliferation, significantly increasing infection risk. In our clinical experience, over two-thirds of patients experience skin involvement related to these immune alterations.
Most concerning is how hyperglycemia simultaneously dulls certain immune responses while overstimulating others. This paradoxical effect explains why you might experience both delayed wound healing and excessive inflammatory reactions in different skin regions—a hallmark of diabetes-related dermatological manifestations.
Prevention Strategies for Maintaining Healthy Skin With Diabetes
For individuals with diabetes, maintaining healthy skin requires a proactive approach that addresses the complex interplay between glucose regulation and dermal integrity. We recognize that consistent blood glucose control forms the foundation of effective preventive measures, as it minimizes inflammation and supports ideal skin function.
Implementing thorough skincare routines tailored to diabetic needs greatly reduces complications. This includes daily cleansing with gentle, fragrance-free products and consistent moisturization with ceramide-rich creams that strengthen the skin barrier. We recommend diligent skin monitoring, particularly of the extremities, to identify potential issues before they escalate.
Incorporating foods rich in zinc and copper can significantly enhance wound healing and maintain skin elasticity, which is particularly beneficial for preventing diabetic skin complications.
Remember that we’re all working together to manage this condition. By combining glucose management with specialized skincare protocols, we can protect your skin’s health and enhance your overall wellbeing.
Treatment Options for Diabetes-Related Skin Complications
When diabetes disrupts normal skin function, an all-encompassing treatment approach becomes essential to manage the resulting complications. We prioritize lifestyle modifications that target insulin resistance—the metabolic root cause of many dermatological manifestations. Weight reduction, optimized glycemic control, and increased physical activity form our foundation for hormonal rebalancing.
For localized conditions, we implement topical treatments strategically. Retinoids reduce epidermal thickness while keratolytic agents containing ammonium lactate address hyperkeratosis. Vitamin D analogs and tacrolimus offer superior anti-inflammatory benefits without skin atrophy risks. For patients with vitiligo, topical steroids combined with proper SPF 30+ sunscreen protection is recommended to manage discolored skin patches.
In our practice, we’ve observed remarkable improvements with combination therapies: metformin or GLP-1 agonists paired with appropriate topicals for acanthosis nigricans, and corticosteroid injections for necrobiosis lipoidica. Together, we’ll develop your personalized protocol to restore skin integrity.
When to Seek Medical Attention for Diabetic Skin Problems
Recognizing the threshold between self-management and necessary medical intervention represents a critical skill for everyone with diabetes-related skin conditions. We recommend immediate medical attention for severe hypoglycemia symptoms with skin pallor, widespread necrosis, or infections with systemic symptoms like fever.
Early intervention markedly improves outcomes for new or changing lesions. Contact your healthcare provider when you notice persistent shin spots, ring-shaped reddish lesions on shins, or orange-yellow nodular deposits under the skin.
We encourage regular skin evaluations for complications like non-healing wounds, infected insulin injection sites, or persistent dry, itchy skin. Remember, those with diabetic dermopathy face higher neuropathy risk. Be especially vigilant about checking areas affected by acanthosis nigricans as these darkened patches in skin folds may indicate poorly controlled diabetes. As your partners in diabetes management, we emphasize that prompt attention to skin changes protects your overall metabolic health.
Frequently Asked Questions
Can Diabetic Skin Conditions Affect Children Differently Than Adults?
Yes, we’ve observed children’s diabetic skin manifestations differ markedly from adults. Childhood eczema from insulin devices is common, while adults face conditions linked to long-term insulin resistance affecting dermal thickness and metabolic pathways.
How Do Seasonal Changes Impact Diabetic Skin Conditions?
We’ve observed that seasonal dryness worsens diabetic skin integrity, while humidity effects alter glucose metabolism. Winter’s cortisol spikes reduce insulin production, and summer’s fluctuating hydration compromises our skin barrier function markedly.
Are Certain Ethnicities More Prone to Specific Diabetic Skin Manifestations?
Yes, we’ve observed significant ethnic disparities in diabetic skin manifestations. African Americans show higher acanthosis nigricans rates (13%) versus whites (0.5%), reflecting differences in skin sensitivity to hyperinsulinemia across our diverse community of patients.
Can Weight Fluctuations Worsen Existing Diabetic Skin Conditions?
Yes, weight fluctuations greatly worsen diabetic skin conditions. We’ve observed how unstable weight patterns disrupt insulin sensitivity, compromising skin integrity. Consistent weight management and ideal skin hydration are essential components of our metabolic homeostasis strategy.
Do Diabetic Skin Complications Differ Between Men and Women?
Yes, we observe that hormonal differences between sexes affect diabetic skin complications. Women’s fluctuating estrogen levels increase skin sensitivity, while men’s higher testosterone influences sebum production and wound healing patterns in our diabetic community.
Conclusion
We’ve seen how diabetes disrupts the skin’s metabolic equilibrium, with insulin resistance triggering inflammatory cascades and compromising dermal integrity. Remember, glycemic control directly correlates with cutaneous health. By maintaining ideal HbA1c levels, implementing consistent hydration, and promptly addressing microbial colonization, you’re preserving not just epidermis integrity but enhancing overall glucose homeostasis. Your skin’s condition often reflects your endocrine system’s functionality—monitor both vigilantly.
